Science news - point of care diagnostics
21-September-2010
Do it yourself
Jon Cooper can remember clearly when he decided to become a scientist, he says. “I was 8 or 9 and we had got this new science lab at my school on the outskirts of London. You had to walk across the playing fields to get to it.
"It was like a different world out there. It always seemed to me that you were leaving school and going somewhere to have fun.”
Now the leader of a large bioengineering research group, Professor Cooper is clearly still  having fun, while doing serious research with important applications. He can only spare twenty minutes, he says at first, because he has another meeting. One hour later he is still talking about the work that engrosses him.
having fun, while doing serious research with important applications. He can only spare twenty minutes, he says at first, because he has another meeting. One hour later he is still talking about the work that engrosses him.
“Engineering and science are about curiosity, creativity and imagination,” he says. “You have to try to think differently from other people.”
The diagnosis and treatment of disease in poor countries is one area where his group of researchers is thinking differently.
Point of care
“Traditionally if you’re not feeling well a doctor will take a blood sample and you will come back a week later to get the result," says Professor Cooper. "What we’re looking at now is point of care testing, where you administer your own medicine based on a test you do yourself – and get the result right away.”
An obvious existing example is the glucose meter, he says. “The person with diabetes is able to respond immediately to the measurement by taking insulin or sugar. So diabetes, which used to kill about 100,000 people a year, can now be managed relatively easily.”
Point of care is particularly vital in poor countries, says Professor Cooper, where infectious diseases are very common and the healthcare systems struggle. “But it’s also important in the poorer parts of developed countries. You get tens of people dying of TB in Glasgow each year, which translates to thousands across the developed world."
Shed in a field
This whole idea of doing diagnostics where you don’t need to go to hospital and are able to "get a reading very quickly" is growing in importance, says Professor Cooper. "In a developing country a field clinic will typically be a shed with a desk and a nurse sitting outside it. Doing diagnosis in those environments is difficult.
"The standard way is to take a blood sample and look at it through a microscope. But keeping a microscope running in those conditions is pretty tricky."
A cheap device that could tell if a blood sample had disease micro-organisms in it would be ideal. But such devices would need to be small and reliable and run on low power. This is a tough set of requirements. It will take imaginative engineering to achieve them.
“We have been looking at using sound waves to do the job," he says.
Making waves
Surface acoustic waves (SAW) is a technology that's already used in mobile phones, bank touch screens and TV tuners, says Professor Cooper. “Your finger gets in the way of the sound waves and the instrument detects that.
"What we’re looking at now is using that same approach in point of care diagnosis. But instead of a finger you put a drop of fluid in the way of the sound wave.
"That gives you a low cost, low power method of moving your fluid sample - which can be blood, urine or saliva.”
But manipulation of the sample is only part of what's needed to do point of care diagnosis. The new devices being developed in Professor Cooper’s group must also be able to analyse and diagnose as well as manipulate. Here too sound waves are the secret, he says.
Parasites
Trypanosome parasites for example are carried in blood and are much larger than red and white blood cells. So they can be detected through their effects on a focused sound wave passing through the sample.
“Malaria is different because the plasmodium that causes it enters the blood cells," says Professor Cooper. "That means we can’t differentiate by size. But we can by using changes in mechanical properties. Red 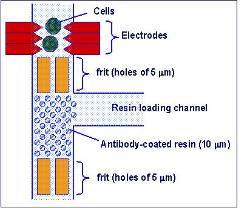 blood cells carrying the parasite are stiffer – which is what causes some of the problems when you have the disease – and again that has an effect on the acoustic wave. So we can measure that.”
blood cells carrying the parasite are stiffer – which is what causes some of the problems when you have the disease – and again that has an effect on the acoustic wave. So we can measure that.”
Other ways of engineering fluids with sound are being developed by Professor Cooper’s large group of bioengineers. These include bursting blood cells open – lysing them – to study what’s inside and setting a small droplet spinning like a miniature centrifuge to separate its contents.
What we do
Professor Cooper's group have also shown that they can make devices with a material that can be thrown away after the test and replaced. "This very much reduces the cost," he says.
"It's a similar model to a disposable razor where you have a nice head and handle, but blades are used and thrown away. It enables you to make cheap, practical devices."
All this is just one area of research in Professor Cooper's bioengineering group, he says. So what exactly is bioengineering? "That's the interface between engineering – electronics, mechanics, materials – and biology," he says.
"It's what we do."
More help with words
| application | average | bacteria | cell | complex | density |
| design | engineering | engineered | experiment | insulin | infection |
| laboratory | membrane | mass | molecule | organ | pancreas |
| protoplasm | protein | structure | symptom | tissue | volume |
For other websites and resources relevant to this science story try the